Atrioventricular Septal Defect (AVSD or AV CANAL)
An AVSD is the most common congenital heart defect found in children with Down's Syndrome, accounting for 50% of the total.
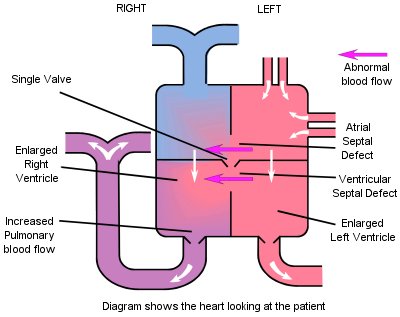
In its complete form there is a hole in the wall between the top chambers (atria) and a hole in the wall between the bottom chambers (ventricles), and one common valve between the two atria and the two ventricles. In the partial forms there may not be a hole between the bottom chambers (ventricles) or the mitral and tricuspid valves may not be joined together, but either or both may leak, known as valve incompetence.
Because of the high pressure in the left ventricle (needed to pump the blood around the body), blood is forced through the holes in the septum (central heart wall) when the ventricle contracts, thus increasing the pressure in the right ventricle. This increased pressure (pulmonary hypertension) results in excess blood flow to the lungs.
Symptoms
Some of the early symptoms which may be exhibited are difficulty in feeding, poor weight gain, fast irregular breathing and a degree of cyanosis (blueness) particularly noticeable around the mouth, fingers and toes. Clinical examination may show an enlarged heart and liver, and a diagnosis of ‘heart failure' may be given. This is not as frightening as it sounds - it is in fact the medical term used to indicate that the heart is working inefficiently due to the demands the body is placing on it. Because of the flow of blood from one side to the other, the heart has to work harder than normal.
Not all children will exhibit symptoms early in life, and those that do will not necessarily show all of these.
Treatment
Early treatment may involve the use of diuretics such as Frusemide and Spironolactone to control the fluid retention around the body and to reduce the volume of blood in the circulation, thus making the heart’s workload easier. These may be used in conjunction with other drugs such as Captopril, to make it easier for blood to pass to the body, rather than back through the hole to the lungs.
Slow weight gain may lead to the addition of additives such as Calogen, Maxijul or Duocal to a baby's milk to increase calorie intake. Severe feeding problems may necessitate feeding by way of a naso-gastric tube (through the nose and directly into the stomach), so that energy is not used up in obtaining nourishment (see Feeding Problems Topic Note).
The majority of cases of AVSD are suitable for surgical intervention; this generally takes place within the first six months of life.
If the condition is left unoperated, the increased blood pressure in the lungs causes damage which eventually makes surgery impossible, as the body adjusts to these pressures and could not cope with the surgery.
Follow up Advice
Often following surgery there remains a leaky valve which requires regular monitoring in case more surgery is needed, although in many cases the heart copes very well with the leakage and no further treatment is required. Sometimes bouts of illness may place an additional strain on the leaky valve, but this may be alleviated by treatment with diuretics for a short period. There may be times when all chest infections require quite energetic treatment. The repeated use of antibiotics, if used properly, is very helpful and does not reduce the child's resistance to infections.
Most children with a cardiac defect, whether repaired or not, no longer require antibiotic cover during any dental treatment. However, good oral hygiene is very important with teeth being brushed twice a day and regular visits to the dentist (see Dental Care for Children and Adults with Heart Problems and Down's Syndrome Topic Note). Body piercing and tattoos also carry a risk of infection and should be avoided if possible. Otherwise, check beforehand with your cardiologist to see if antibiotic cover is required and make sure you go to a reputable practitioner with excellent hygiene standards.